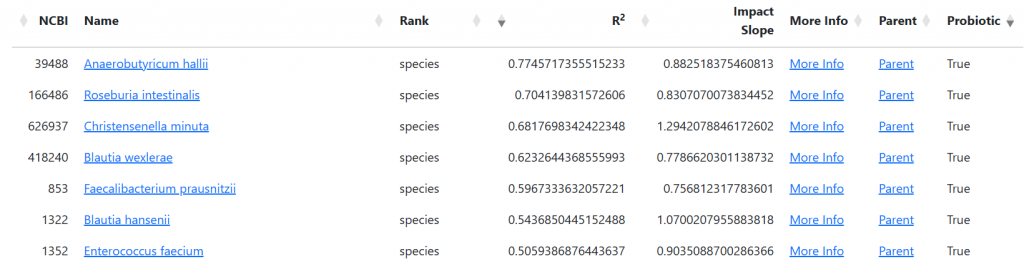
This is just presenting the tables for Autism derived from the methodology described in this technical post: Odds Ratios and the Microbiome. There are only two symptoms with sufficent data to compute odds ratios. If you us Biomesight, make sure your samples have symptoms entered!
Here are some odds ratios using BiomeSight data. Odds Low means when the reading is below the Median and Odds High above the Median (of those with this symptom). We use the symptom median to get balanced (same approximate size) categories. Using an average results in poorer results.
This is recommended reading:Microbiome Statistics for Dummies
- Some bacteria occur less often with Autism, but the average may be the same or higher
- This does no factor in Occurrence Odds Ratios which is critical for some bacteria (like Bifidobacterium)
Official Diagnosis: Autism
The key feature is too much bifidobacterium, to see things that may reduce is see Bifidobacterium Modifiers:
| Tax_Name | tax_Rank | Odds Low | Odds High |
| Bifidobacterium | genus | 0.63 | 2.41 |
| Actinomycetota | phylum | 0.64 | 2.29 |
| Bifidobacteriaceae | family | 0.65 | 2.24 |
| Bifidobacteriales | order | 0.65 | 2.24 |
| Bifidobacterium catenulatum | species | 0.67 | 2.13 |
| Actinomycetes | class | 0.67 | 1.97 |
| Bacteroides rodentium | species | 1.86 | 0.68 |
| Phocaeicola paurosaccharolyticus | species | 1.83 | 0.68 |
| Bifidobacterium gallicum | species | 0.69 | 1.83 |
| Phocaeicola sartorii | species | 1.71 | 0.70 |
| Bifidobacterium catenulatum PV20-2 | strain | 0.71 | 1.70 |
| Phascolarctobacterium succinatutens | species | 1.65 | 0.71 |
| Clostridium thermosuccinogenes | species | 1.59 | 0.67 |
| Pseudoclostridium | genus | 1.59 | 0.67 |
| Bacteroides cellulosilyticus | species | 1.59 | 0.71 |
| Johnsonella | genus | 1.59 | 0.73 |
| Sarcina maxima | species | 0.75 | 1.59 |
| Sarcina | genus | 0.75 | 1.59 |
| Johnsonella ignava | species | 1.59 | 0.73 |
| Bifidobacterium indicum | species | 0.74 | 1.58 |
| Veillonella montpellierensis | species | 0.75 | 1.54 |
| Acidaminococcus | genus | 1.54 | 0.69 |
| Sphingobacteriaceae | family | 1.52 | 0.74 |
| Segatella | genus | 0.75 | 1.52 |
| Hathewaya | genus | 1.52 | 0.74 |
| Phocaeicola | genus | 1.52 | 0.75 |
| Hathewaya histolytica | species | 1.52 | 0.74 |
| Anaerovibrio | genus | 1.50 | 0.74 |
| Rhodothermota | phylum | 1.50 | 0.71 |
| Rhodothermales | order | 1.50 | 0.71 |
| Rhodothermia | class | 1.50 | 0.71 |
| Segatella copri | species | 0.76 | 1.49 |
| Actinomycetaceae | family | 0.77 | 1.49 |
| Porphyromonas | genus | 1.48 | 0.74 |
| Enterobacterales | order | 0.76 | 1.47 |
| Natronincola | genus | 0.76 | 1.47 |
| Sphingobacterium bambusae | species | 1.47 | 0.75 |
| Enterobacteriaceae | family | 0.76 | 1.46 |
| Escherichia | genus | 0.76 | 1.46 |
| Bacteroides finegoldii | species | 1.45 | 0.76 |
| Anaerovibrio lipolyticus | species | 1.45 | 0.76 |
| Natronincola peptidivorans | species | 0.77 | 1.45 |
| Peptostreptococcaceae | family | 0.77 | 1.44 |
| Bifidobacterium choerinum | species | 0.77 | 1.44 |
| Parabacteroides goldsteinii | species | 1.44 | 0.77 |
| Acetobacterium | genus | 1.43 | 0.77 |
| Erysipelothrix | genus | 1.43 | 0.75 |
| Collinsella aerofaciens | species | 0.77 | 1.43 |
| Bifidobacterium adolescentis | species | 0.78 | 1.42 |
| Phocaeicola massiliensis | species | 1.42 | 0.73 |
| Acetivibrio | genus | 1.42 | 0.77 |
| Streptococcus australis | species | 0.79 | 1.41 |
| Streptococcus parasanguinis | species | 0.78 | 1.41 |
| Candidatus Amoebophilus | genus | 1.41 | 0.76 |
| Candidatus Amoebophilus asiaticus | species | 1.41 | 0.76 |
| Amoebophilaceae | family | 1.41 | 0.76 |
| Selenomonas | genus | 1.40 | 0.77 |
| Desulfovibrio | genus | 1.40 | 0.77 |
| Caloramator fervidus | species | 1.40 | 0.76 |
| Anaerotruncus | genus | 1.39 | 0.78 |
| Bacteroides faecis | species | 1.38 | 0.78 |
| Acetivibrio alkalicellulosi | species | 1.37 | 0.78 |
| Selenomonas infelix | species | 1.37 | 0.77 |
| Clostridium | genus | 1.37 | 0.79 |
| Actinomyces | genus | 0.80 | 1.36 |
| Bacteroides fragilis | species | 0.79 | 1.36 |
| Erysipelothrix muris | species | 1.36 | 0.78 |
| Alkalithermobacter thermoalcaliphilus | species | 0.80 | 1.35 |
| Anaerotruncus colihominis | species | 1.35 | 0.79 |
| Sphingobacteriales | order | 1.34 | 0.80 |
| Sphingobacteriia | class | 1.34 | 0.80 |
| Caloramator | genus | 1.33 | 0.80 |
| Bifidobacterium longum | species | 0.80 | 1.33 |
| Caloramator mitchellensis | species | 1.32 | 0.80 |
| Peptococcus | genus | 1.32 | 0.79 |
| Coprococcus eutactus | species | 0.81 | 1.32 |
| Rhodocyclales | order | 0.82 | 1.32 |
| Acidaminococcales | order | 1.31 | 0.81 |
| Acidaminococcaceae | family | 1.31 | 0.81 |
| Faecalibacterium prausnitzii | species | 1.30 | 0.81 |
| Veillonella | genus | 0.82 | 1.30 |
| Peptococcus niger | species | 1.29 | 0.80 |
| Oscillospira | genus | 1.29 | 0.81 |
| Streptococcus | genus | 0.82 | 1.29 |
| Ruminococcus callidus | species | 0.82 | 1.29 |
| Blautia | genus | 1.29 | 0.82 |
| Anaerostipes | genus | 1.29 | 0.81 |
| Serratia | genus | 0.82 | 1.28 |
| Streptococcaceae | family | 0.82 | 1.28 |
| delta/epsilon subdivisions | clade | 1.28 | 0.82 |
| Phocaeicola vulgatus | species | 1.28 | 0.82 |
| Peptostreptococcaceae incertae sedis | no rank | 0.82 | 1.28 |
| Caldicellulosiruptoraceae | family | 1.27 | 0.82 |
| Caldicellulosiruptorales | order | 1.27 | 0.82 |
| Caldicellulosiruptor | genus | 1.27 | 0.82 |
| Sedimentibacter hydroxybenzoicus | species | 1.27 | 0.82 |
| unclassified Bacteroidetes Order II. | order | 1.27 | 0.79 |
| Deltaproteobacteria | class | 1.27 | 0.82 |
| Coriobacteriia | class | 0.83 | 1.27 |
| Burkholderiaceae | family | 0.86 | 1.27 |
| Haemophilus parainfluenzae | species | 0.83 | 1.27 |
| Ectothiorhodospiraceae | family | 1.26 | 0.81 |
| Collinsella | genus | 0.83 | 1.26 |
| Clostridiaceae | family | 1.26 | 0.83 |
| Streptococcus thermophilus | species | 0.84 | 1.26 |
| Phascolarctobacterium | genus | 1.26 | 0.83 |
| Shewanellaceae | family | 1.26 | 0.79 |
| Shewanella | genus | 1.26 | 0.79 |
| Desulfovibrionales | order | 1.26 | 0.82 |
| Desulfovibrionia | class | 1.26 | 0.82 |
| Peptoniphilaceae | family | 1.26 | 0.83 |
| Yersiniaceae | family | 0.84 | 1.26 |
| Porphyromonas canis | species | 1.26 | 0.77 |
| Nostocaceae | family | 1.26 | 0.82 |
| Odoribacter | genus | 1.25 | 0.82 |
| Carnobacteriaceae | family | 0.86 | 1.25 |
| Tissierellales | order | 1.25 | 0.83 |
| Nitrosomonadales | order | 0.88 | 1.25 |
| Pasteurellales | order | 0.84 | 1.24 |
| Pasteurellaceae | family | 0.84 | 1.24 |
| Serratia entomophila | species | 0.84 | 1.24 |
| Parabacteroides merdae | species | 1.24 | 0.84 |
| Desulfovibrionaceae | family | 1.24 | 0.84 |
| Rhodothermaceae | family | 1.24 | 0.83 |
| Thermoanaerobacterales Family III. Incertae Sedis | family | 1.23 | 0.82 |
| Bacteroides graminisolvens | species | 0.86 | 1.23 |
| Sporomusaceae | family | 1.23 | 0.81 |
| Bacteroides stercorirosoris | species | 1.23 | 0.84 |
| Parabacteroides johnsonii | species | 1.23 | 0.82 |
| Bacteroides thetaiotaomicron | species | 1.23 | 0.84 |
| Haemophilus | genus | 0.85 | 1.23 |
| Alphaproteobacteria | class | 1.23 | 0.84 |
| Hydrocarboniphaga daqingensis | species | 1.23 | 0.81 |
| Pectinatus cerevisiiphilus | species | 0.85 | 1.23 |
| Bacteroides | genus | 1.22 | 0.85 |
| Eubacteriaceae | family | 1.22 | 0.84 |
| Lactobacillus | genus | 0.85 | 1.22 |
| Paraprevotella clara | species | 1.22 | 0.82 |
| Olivibacter | genus | 1.22 | 0.85 |
| Dorea | genus | 1.22 | 0.85 |
| Peptoniphilus | genus | 1.22 | 0.84 |
| Peptoniphilus methioninivorax | species | 1.22 | 0.85 |
| Pseudomonadota | phylum | 0.85 | 1.22 |
| Lachnospiraceae | family | 1.22 | 0.85 |
| Butyrivibrio | genus | 1.21 | 0.82 |
| Blautia coccoides | species | 1.21 | 0.85 |
| Butyrivibrio proteoclasticus | species | 1.21 | 0.82 |
| Oscillospira guilliermondii | species | 1.21 | 0.85 |
| Rhodothermus | genus | 1.21 | 0.84 |
| Bacteroides uniformis | species | 1.21 | 0.85 |
| Rhodothermus clarus | species | 1.21 | 0.84 |
| Hyphomicrobiales | order | 1.21 | 0.74 |
| Pectinatus | genus | 0.86 | 1.21 |
| Pedobacter | genus | 1.20 | 0.85 |
| Ruminiclostridium cellobioparum | species | 1.20 | 0.85 |
| Ruminiclostridium cellobioparum subsp. termitidis | subspecies | 1.20 | 0.85 |
Autism: High Functioning
There is stark contrast with the above, bifidobacterium is not seen in the top ones!
| Tax_Name | tax_Rank | Odds Low | Odds High |
| Desulfovibrionales | order | 0.677395 | 2.024324 |
| Desulfovibrionia | class | 0.677395 | 2.024324 |
| Desulfovibrionaceae | family | 0.678547 | 2.013471 |
| Dorea | genus | 1.814651 | 0.677811 |
| Bilophila | genus | 0.708843 | 1.779777 |
| Anaerotruncus colihominis | species | 0.702471 | 1.734749 |
| Deltaproteobacteria | class | 0.72187 | 1.689058 |
| Phocaeicola | genus | 1.669274 | 0.70199 |
| delta/epsilon subdivisions | clade | 0.725986 | 1.665663 |
| Sphingobacterium | genus | 0.728026 | 1.654401 |
| Sphingobacteriaceae | family | 0.72872 | 1.650617 |
| Anaerotruncus | genus | 0.74642 | 1.618626 |
| Odoribacter | genus | 0.729266 | 1.590437 |
| Anaerofilum | genus | 0.754147 | 1.527128 |
| Holdemania | genus | 0.745745 | 1.517317 |
| Bacteroides thetaiotaomicron | species | 0.749716 | 1.50114 |
| Sphingobacterium shayense | species | 0.763319 | 1.494186 |
| Porphyromonadaceae | family | 0.770477 | 1.46075 |
| Parabacteroides | genus | 0.771714 | 1.456064 |
| Tannerellaceae | family | 0.771714 | 1.456064 |
| PVC group | clade | 0.761649 | 1.455481 |
| Verrucomicrobiota | phylum | 0.762716 | 1.451602 |
| Odoribacteraceae | family | 0.762844 | 1.451138 |
| Bacillales incertae sedis | no rank | 1.447434 | 0.753405 |
| Lachnospiraceae | family | 1.447185 | 0.753477 |
| Chromatiales | order | 0.795258 | 1.44706 |
| Parabacteroides merdae | species | 1.446031 | 0.764263 |
| Rhodothermia | class | 1.440393 | 0.744067 |
| Rhodothermota | phylum | 1.440393 | 0.744067 |
| Rhodothermales | order | 1.440393 | 0.744067 |
| Flavobacteriia | class | 0.787583 | 1.440238 |
| Flavobacteriales | order | 0.787583 | 1.440238 |
| Flavobacteriaceae | family | 0.787583 | 1.440238 |
| Sphingobacteriia | class | 0.778414 | 1.43145 |
| Sphingobacteriales | order | 0.778414 | 1.43145 |
| Thiotrichaceae | family | 1.414958 | 0.737403 |
| Blautia obeum | species | 1.400871 | 0.767464 |
| Caloramator fervidus | species | 0.788721 | 1.400038 |
| Parabacteroides distasonis | species | 0.789546 | 1.393203 |
| Eubacterium | genus | 0.78004 | 1.39273 |
| Burkholderiaceae | family | 0.794255 | 1.379749 |
| Bacteroides stercoris | species | 1.376547 | 0.775412 |
| Lactobacillales | order | 1.37481 | 0.775997 |
| Peptococcus | genus | 1.372916 | 0.776637 |
| Bacilli | class | 1.368623 | 0.778099 |
| Paraprevotella | genus | 1.356618 | 0.747396 |
| Tindallia magadiensis | species | 0.791961 | 1.356281 |
| Tissierellia | class | 1.351294 | 0.784153 |
| Anaerostipes | genus | 1.349608 | 0.784169 |
| Hathewaya histolytica | species | 0.804359 | 1.346859 |
| Hathewaya | genus | 0.804985 | 1.345006 |
| Bacillales | order | 1.344775 | 0.786496 |
| Peptococcus niger | species | 1.343812 | 0.786845 |
| Phocaeicola paurosaccharolyticus | species | 1.342696 | 0.796668 |
| Blautia coccoides | species | 1.34018 | 0.788169 |
| Coprococcus | genus | 1.324735 | 0.793933 |
| Anaerovibrio | genus | 0.818323 | 1.308705 |
| Pseudomonadota | phylum | 0.820638 | 1.3011 |






Recent Comments